The International and Multi-Regional Membership Center of Latinos in the USA
Welcome to you all!



Are We Seeing a Diabetes Epidemic in the USA?
PuraVidaCommunity

As of April 30, 2016, the United States has a total resident population of 323,730,000, making it the third most populous country in the world. It is very
urbanized, with 81% residing in cities and suburbs as of 2014 (the worldwide urban rate is 54%). Of the almost 324 million people in the nation, More than
29 million people in the United States have diabetes, up from the previous estimate of 26 million in 2010, according to a report released today by the
Centers for Disease Control and Prevention. One in four people with diabetes doesn’t know he or she has it. These figures represent close to a 10.8% of
the population of the nation suffers diabetes, and the numbers are steadily growing.
Another 86 million adults – more than one in three U.S. adults – have pre-diabetes, where their blood sugar levels are higher than normal but not high
enough to be classified as type 2 diabetes. Without weight loss and moderate physical activity, 15 percent to 30 percent of people with pre-diabetes will
develop type 2 diabetes within five years.
Key findings from the National Diabetes Statistics Report, 2014 (based on health data from 2012), include:
•
29 million people in the United States (9.3 percent) have diabetes.
•
1.7 million people aged 20 years or older were newly diagnosed with diabetes in 2012.
•
Non-Hispanic black, Hispanic, and American Indian/Alaska Native adults are about twice as likely to have diagnosed diabetes as non-Hispanic white
adults.
•
208,000 people younger than 20 years have been diagnosed with diabetes (type 1 or type 2).
•
86 million adults aged 20 years and older have pre-diabetes.
•
The percentage of U.S. adults with pre-diabetes is similar for non-Hispanic whites (35 percent), non-Hispanic blacks (39 percent), and Hispanics (38
percent).

More alarming is that over 95 percent of these suffer from a “self-inflicted” form known as Type 2.
Looking at the Problem
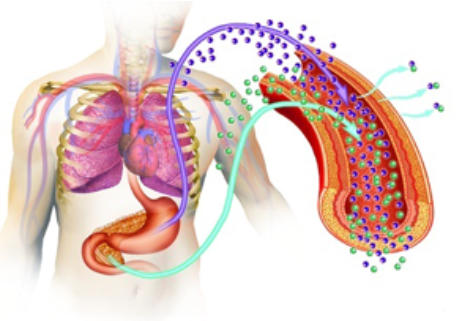
To better appreciate this condition, one must first understand the hormone insulin. According to EndocrineWeb: “Insulin is a hormone made by the
pancreas that allows your body to use sugar (glucose) from carbohydrates in the food that you eat for energy or to store glucose for future use. Insulin
helps [keep] your blood sugar level from getting too high (hyperglycemia) or too low (hypoglycemia).
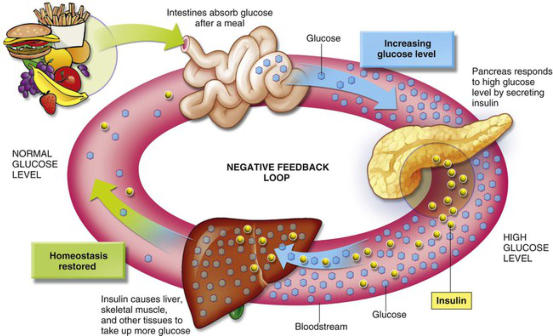
“The cells in your body need sugar for energy. However, sugar cannot go into most of your cells directly. After you eat food and your blood sugar level
rises, cells in your pancreas (known as beta cells) are signaled to release insulin into your bloodstream. Insulin then attaches to and signals cells to absorb
sugar from the bloodstream. Insulin is often described as a ‘key,’ which unlocks the cell to allow sugar to enter the cell and be used for energy.”
Insulin production is involved in the two types of diabetes, yet there is a difference between them.
Type 1: Also known as insulin-dependent diabetes, this condition is almost always
hereditary and afflicts most before the age of 20. Even those with the best habits and
health are not safe from this genetic condition.
Almost all of us have seen or known someone who had to take daily shots of insulin or, in
more recent years, has worn an insulin pump to periodically administer it. This is necessary
because Type 1 diabetics do not produce sufficient amounts of insulin (or potentially any
at all) in the pancreas.
Type 2: Again, this is known adult onset diabetes. Those who have it actually continue to
produce insulin. In many cases, a person’s pancreas may even produce too much. Yet the
body is unable to recognize the insulin and use it properly.
This is known as insulin resistance. Some insulin resistance is natural over the course of a
lifetime for the average person, however, Type 2 diabetes greatly accelerates insulin
resistance.
Why are both forms of diabetes so problematic? Simple. When your body either fails to produce or recognize insulin, sugar cannot get into your cells and
instead builds up in your blood.
This is dangerous for two reasons.
First, since sugar cannot get into the cells, the cells cannot use the sugar to produce energy.
Second, excessive blood sugar damages and eventually destroys blood vessels, which can result in lower leg amputations, blindness and kidney failure,
the latter forcing a person onto dialysis for the remainder of his life.
Caused by Sugar
To understand the real epidemic, revisit the fact that 95 percent of diabetics have Type 2 diabetes—which is a self-inflicted kind!
There are multiple contributing factors to developing this disease such as
inactivity, over consumption of food, and obesity. But it is almost universally
accepted that the over consumption of sugar, specifically, is one of the primary
causes.
Yet sugar is in healthy foods such as honey and fruit. So, it cannot be all bad,
right? Yes and no.
Consider the following from Everyday Health: “The sugars in food are known as
simple carbohydrates and are a natural component of many fresh foods, such
as the lactose in milk and the fructose in fruits. A healthy, well-balanced diet
will always have these sugars in it.“
However, the problem with sugar is the sheer amount of it that’s in the typical
American diet. Added sugars—the sucrose in table sugar as well as the sugars in
foods such as sodas, cereals, packaged foods, and snacks—when consumed in
excess, cause weight gain, heart disease, mood swings, and more.
“Research has found that a high-sugar diet certainly increases diabetes risk—adding just one serving of a sweetened beverage each day to your diet ups
risk by 15 percent, a study at the Harvard School of Public Health found…”
So just how much sugar and foods with sugar are Americans consuming? According to the United States Department of Agriculture, the average American
consumes 130 pounds of refined sugars per year. This comes out to 160 grams—about a third of a pound of sugar—per day.
While it may seem as though there is no way a person could consume that much, keep in mind that this is an average! This means that there are some
people who only consume 20-30 pounds of sugar and some who consume 300 or more pounds of sugar per year—almost a POUND PER DAY!
Solution - Go back to basics a traditional way of life
With such an epidemic level of sugar consumption, it seems the best solution would be to say, “Stop eating sugar.” This would certainly be a huge step in
the right direction, especially considering that less than 100 years ago, the average intake of sugar was only about four pounds per year and levels of Type 2
diabetes were almost non-existent.
But a slightly more in-depth explanation may provide a better understanding of what
you can do and how different our diet is today compared to generations past.
There are two factors in which the diet of the past 6,000 years differs from that of
today.
Historically, people did eat large amounts of carbohydrates and some sugar, but these
were in the form of complex (slow-burning) carbohydrates such as sweet potatoes and
whole grains including oatmeal, millet and flax.
Second, life in general was an exercise in stamina. Most people worked in agriculture or
had jobs that required large amounts of physical labor. The carbohydrates people
consumed not only entered their bloodstreams more slowly, but they burned them
quickly due to high levels of activity.
Since this was the case, people generally never experienced a blood sugar spike, which
would have resulted in the need for large amounts of insulin.
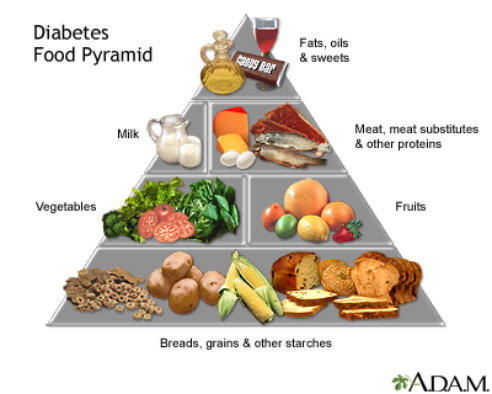
With that in mind, the solution is simple: If you want to avoid falling prey to Type 2 diabetes, stay active. Eat simple foods from the food pyramid—lean
meats, whole grains, lots of vegetables, and a few fruits in the absence of soda, sugary treats, and snack foods.
Just making these small changes goes a long way in preventing this self-inflicted and preventable disease!

Diabetes Among Hispanics
People of Hispanic and Latino origin are at high risk for developing type 2 diabetes and related cardiometabolic abnormalities, but the risk varies
considerably among specific ethnic groups and other factors, such as the length of time they have been living in the United States, according to two
studies and an accompanying commentary being published in the August issue of Diabetes Care®.
A separate study also published in the August issue found that job strain is a risk factor for type 2 diabetes in both men and women, independent of
lifestyle factors.
Researchers have long known that people of Hispanic/Latino background are at higher risk for type 2 diabetes than non-Hispanic Caucasians. However,
most research has looked at this group as a whole, rather than as a number of different populations.
There are more than 50 million Hispanics/Latinos currently living in the United States, making up about 16 percent of the population. The U.S. Census
Bureau estimates that by 2050, one in three people living in the United States will be of Hispanic/Latino origin, including such diverse subgroups as
Puerto Rican, Mexican, Cuban, Central and South Americans. But, wrote the authors of a commentary being published in this issue of Diabetes Care, “the
differences in diabetes and obesity prevalence among Latino subgroups are masked when all individuals are combined into a single group.”
The Hispanic Community Health Study/Study of Latinos (HCHS/SOL) was launched by the National Heart, Lung and Blood Institute in part to fill in
knowledge gaps regarding the prevalence and development of chronic diseases, such as diabetes, among the diverse members of these populations. It
found considerable diversity among Hispanic/Latino groups when it comes to the prevalence of diabetes, as well as a low rate of diabetes awareness,
diabetes control and health insurance.
Important Links


